OE Express from Workforce Junction
Are you a Benefits Advisor under pressure? Let’s turn pressure into profit!
With a turnkey deployment of an enterprise-grade enrollment platform.
A client-branded enrollment portal enhances the value proposition of employee benefits!
Are you still using paper enrollments for your smaller groups?
Click here to check out the 24 plus advantages of using an online self-service system.Talk to us about the return on investment for the benefit advisor and the employer.
Risk Free
Our money back guarantee makes it incredibly easy for you to try us for the first time (or to try us again). If your don’t realize ROI at least equal to the deployment fee, we’ll return the fee in full.
Stop Doing It In House!
Focus your energy on client relationships and leave the ‘dirty work’ to us.
We offer many more services to support you, in addition to deploying custom branded portals.
It’s never too late to turn OE pressure into profit
It only takes 10 minutes to find out more… or get started. Simply use the link below to set up a time that is convenient for you.
Schedule your free initial consultation today!
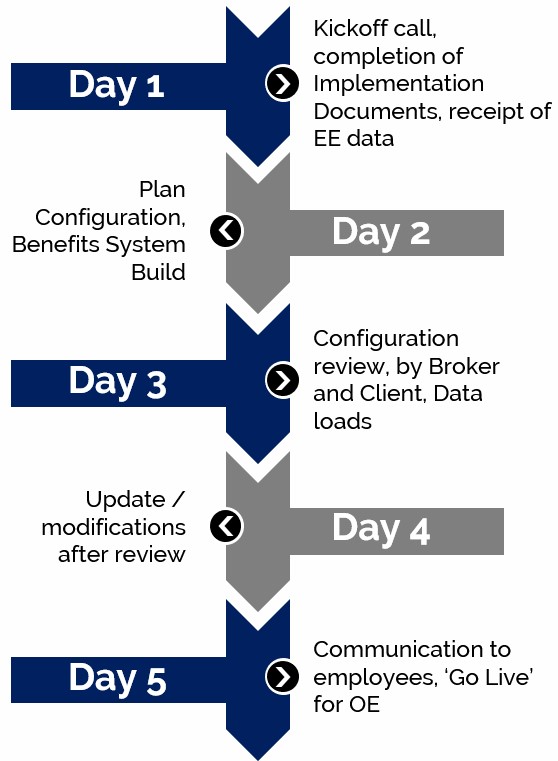
Go Live In Five
"I can say from experience the promise of 'go live in five' is true! Get them the info they need, be ready to review the set up in 2 – 3 days, then go live to employees in 5. It’s a far better option than all that time and effort doing it yourself!"
Jennifer Carroll, HIA
Benefits Systems Administrator
TrueNorth Companies
YOUR CUSTOMER SUCCESS TEAM

Implementation Manager �
Acts as the liaison between the benefit advisor, their employer clients, and Workforce Junction team. Oversees all activity and advocates on your behalf when and where necessary.

Configuration Team �
Ensures Benefits Junction is accurately configured to meet all requirements and preferences of the employer. �
Solution Architects
Our team of subject matter experts (Product, Automation, Communications, Process Development, Technology Integrations) review problems, develop solutions, and “make the complex simple”. � �